Stress Fracture: Diagnosis, treatment and prevention
“You have a stress fracture.”

Just the thought will make most long distance runners cringe. As Dr. Davis puts it, “This is one of the few ailments that I encounter with my endurance athletes that requires immediate attention. It is never easy to tell a lifelong distance runner that they have to shut things down for a while. Pain is a familiar aspect of distance running, but fortunately most patients recognize that the pain related to a stress fracture is distinctly different.”
What is a stress fracture?
A stress fracture is an overuse injury. It occurs when muscles become fatigued and are unable to absorb added shock. It is the loss of the protective role of the muscle that leads to added stress within the bone. Healthy bone continuously undergoes a process called remodeling, which involves replacing old or damaged bone with new healthy bone. Because the body is unable to keep up with the accumulating damaged bone, eventually a tiny crack called a stress fracture develops. “I use the analogy of the scales of justice when discussing stress fractures with patients. Understanding that running causes an imbalance, which leads to accumulation of damage, and ultimately a stress fracture. Knowing that rest is the only way to heal this damage helps most patients come to terms with the need to take a break from running.”
How does it occur?
Though distance running is associated with stress fractures, other risk factors also play a role. Improper training habits, such as increasing the amount or intensity of an activity too rapidly, are common risk factors. They also can be caused by the impact of an unfamiliar surface (a tennis player who has switched surfaces from a soft clay court to a hard court).
Dr. Davis notes, “I see this commonly as we transition from the cold winter months into the warmth of spring. Many runners are excited about the warmer weather and go from running on the shock absorbing treadmill surface to the hard pavement. Unfortunately, the bone is not able to adapt quickly, and stress fractures occur”. Improper equipment such as wearing old or worn shoes that have lost their shock absorbing ability is also a common issue.
Most stress fractures occur in the weightbearing bones of the lower leg and the foot. More than 50 percent of all stress fractures occur in the lower leg.
Stress fractures are not limited to distance runners. Studies have shown that athletes participating in tennis, track and field, gymnastics, and basketball are very susceptible to
stress fractures.
What is the Female Athlete Triad?

Medical studies have shown that female athletes seem to experience more stress fractures than their male counterparts. Dr. Davis states, “This is certainly multifactorial. We acknowledge that our female athletes tend to have less protective muscle mass. But other factors such as diet, decreased bone density and hormonal changes are also involved”. Traditionally, this has been referred to as “the female athlete triad”: eating disorders (bulimia or anorexia), amenorrhea (infrequent menstrual cycle), and osteoporosis (decreased bone density). As a female’s bone mass decreases, her chances of getting a stress fracture increase. “When discussing this issue with my young female athletes, I try to implore them to think of their bone density similar to a savings or retirement account. The more they are able to build up, or save, if you will, while they are young, the greater reserve they will have later in life”.
What are the symptoms?
The most common complaint associated with a stress fracture is pain with activity. Furthermore, unlike some other overuse conditions such as tendinitis or plantar fasciitis, stress fractures tend to become more painful as the activity continues. Though the pain generally subsides with rest, if left untreated, it is not uncommon for the symptoms to occur with daily activities or while resting.
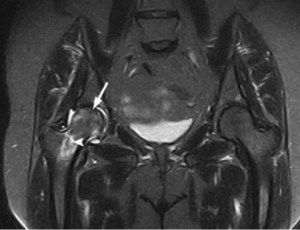
How is it diagnosed?
The medical examination of patients suspected of having a stress fracture generally involves plain radiographs, as well as advance imaging studies such as MRI, bone scan and/or CT scan. Also, depending on individual patient risk factors, the doctor may elect to obtain laboratory test and DEXA bone mineral density study.
How is it treated?
Treatment of stress fractures begins with rest. As Dr. Davis puts it, “the rest is relative. The key is to avoid activities that cause pain. But also recognizing that deconditioning leads to loss of muscle mass, which can lead to recurrence.” Patients often begin a period of activity modifications focusing on low impact exercises. “I frequently refer patients to physical therapy during this phase to address areas of muscle weakness as well as to correct potential issues of improper technique.” The average healing time for stress fractures is 6-8 weeks. In addition to rest, orthotics or braces may be used to help these injuries heal. Occasionally, surgical treatment is necessary, especially with fractures that involve the hip as well as non-healing fractures, which can appear as a “dreaded black line” on plain radiographs.
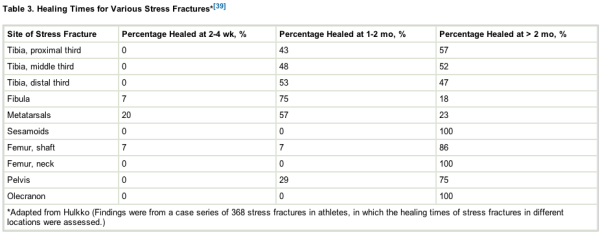
Stress fracture healing time
It is important to remember, early recognition and appropriate treatment are keys to allowing the athlete to return to sports after being diagnosed with a stress fracture.
STRESS FRACTURE PREVENTION STRATEGIES :
- Set incremental goals and gradually build up your mileage on a weekly basis.
- Cross-training alternating activities such as running, rowing and cycling.
- Add strength training and flexibility exercises into the mix.
- Maintain a healthy diet. Make sure you incorporate calcium- and vitamin D-rich foods in your meals.
- Use the proper equipment. Do not wear old or worn running shoes.
- If pain or swelling occurs, immediately stop the activity and rest for a few days. If pain persists, see a physician.